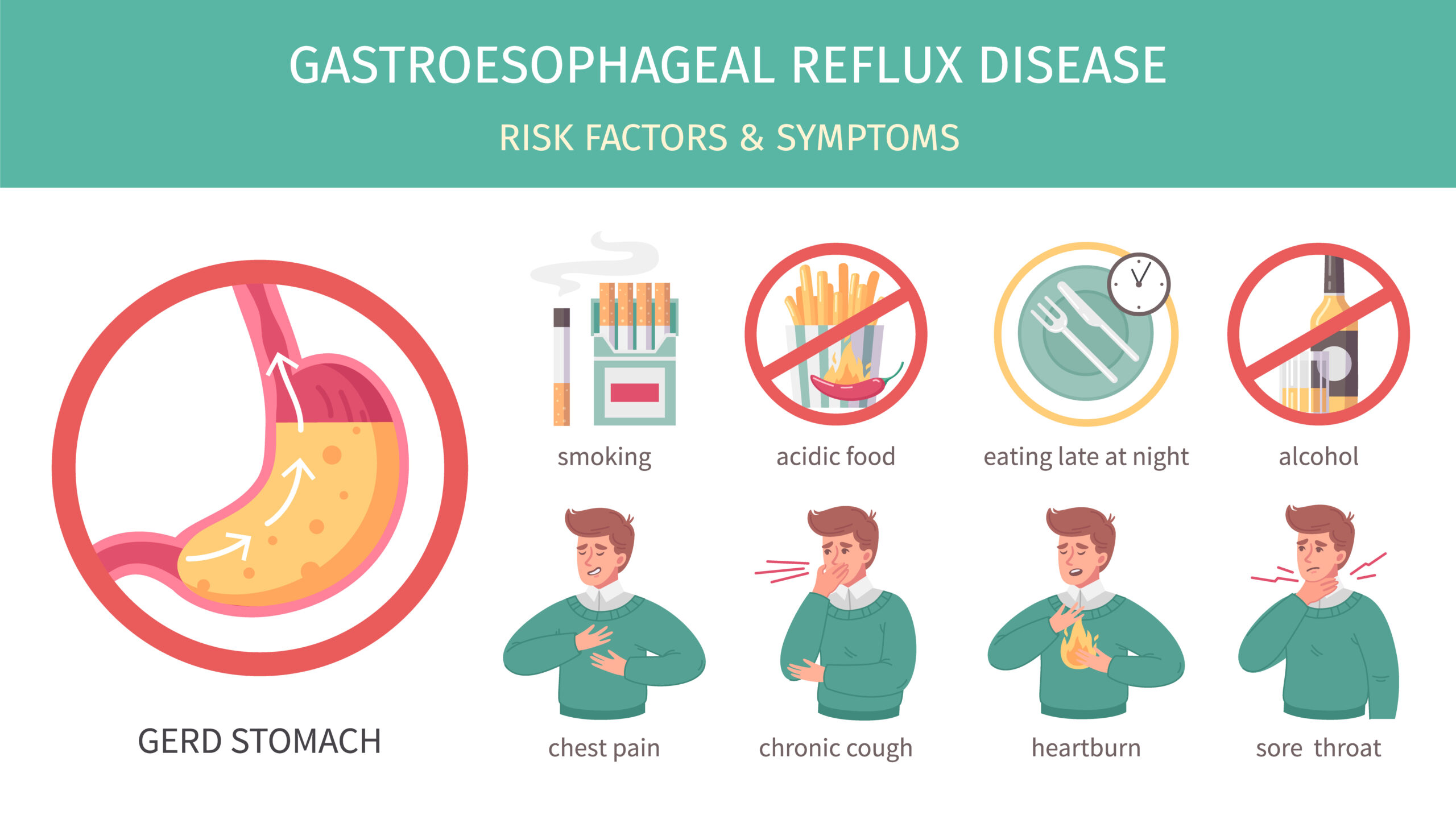
Gastroesophageal Reflux Disease (GERD)
October 15, 2020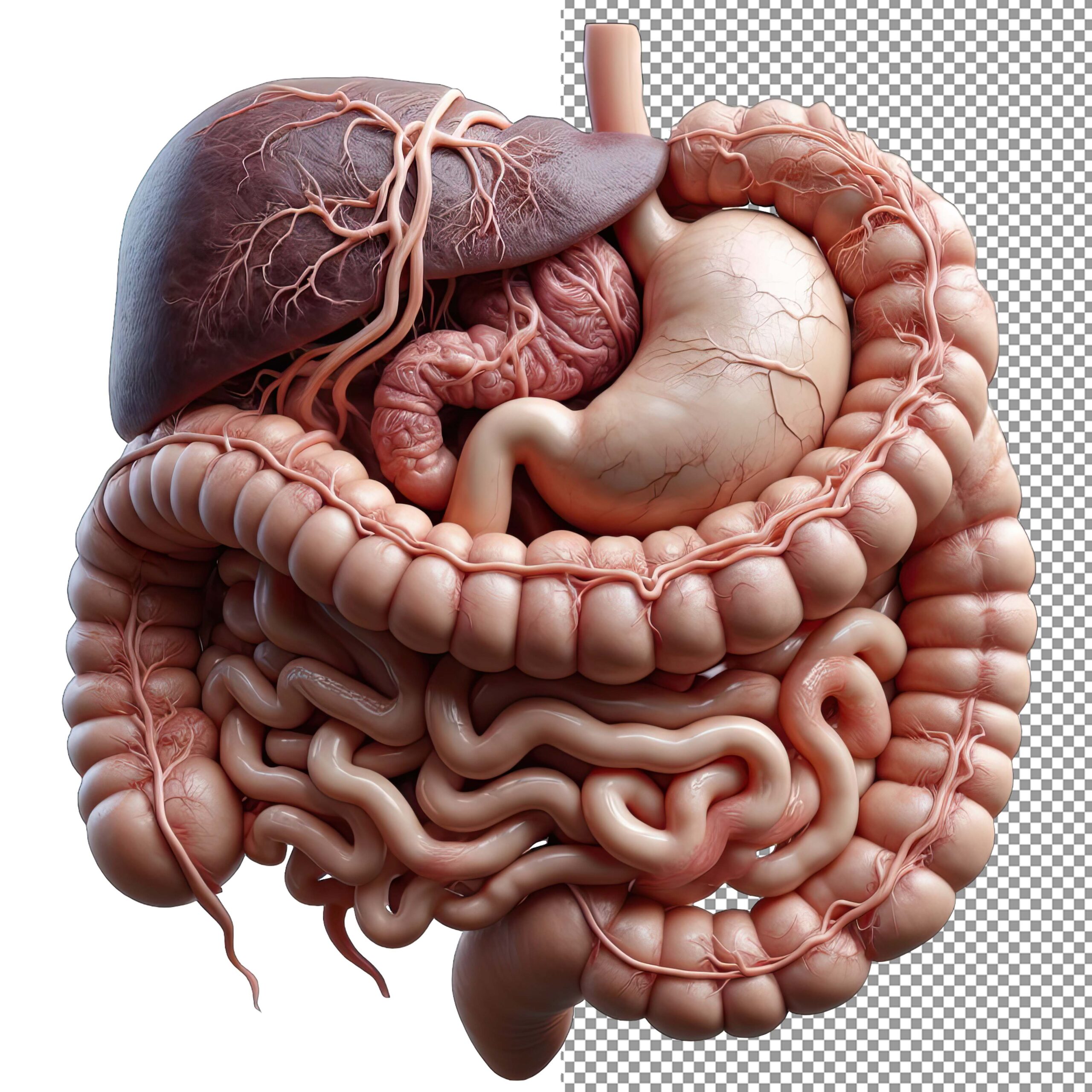
Abdominal Wall
October 16, 2020Paracentesis is a commonly performed beside procedure by which peritoneal fluid is obtained from the peritoneal cavity. This procedure is performed in patients with ascites for diagnostic and/or therapeutic reasons.
Yet, Emergency physicians perform abdominal paracentesis both for a diagnostic sampling of peritoneal fluid and for therapeutic drainage of symptomatic large volume ascites. Ultrasound-guided paracentesis can potentially improve safety and procedural success.
Which Ultrasound Scanner is best for the Paracentesis assessment?
Since a low-frequency transducer 3.5 to 5 MHz is needed for Paracentesis assessment, the Wireless Color Doppler Convex Ultrasound Scanner CC-3.1 is highly recommended to our emergency physicians clients. In which it allows the practitioner to visualize the largest pocket of fluid, increasing procedure success.
Although paracentesis using the traditional landmark technique is generally safe, ultrasound allows visualization of abnormal anatomy to avoid, the deepest pocket of peritoneal fluid, and confirmation that the etiology of abdominal distention is ascites rather than another disease process. Besides, it is easy to use. Ultrasound detection of as little as 100 mL makes it the gold standard for diagnosing ascites.
Furthermore, the ultrasound probe can also be employed in unstable patients with a positive FAST exam. It may be used statically to mark the entry site prior to paracentesis or dynamically to observe the needle entering the peritoneal cavity. The latter is helpful for smaller fluid collections.
To sum up, Ultrasound may be used statically for paracentesis to mark the largest pocket of ascitic fluid or used dynamically for small fluid collections, increasing procedural success. It may also be used to identify anatomic structures to avoid.
References: Ultrasound-Guided Paracentesis